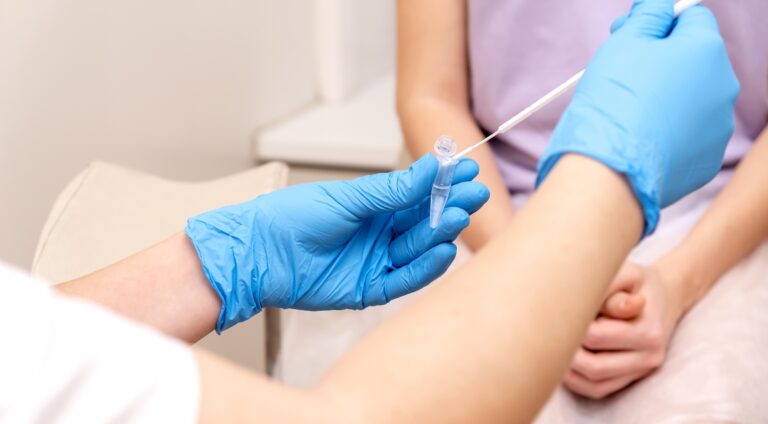
Casual sexual encounters, or one-night stands, are a common experience for many individuals to take part in at least once in their lifetimes. Having a one-night stand can be exciting, but it can also put your health at serious risk, potentially spreading sexually transmitted...
Read More