The question of genital warts vs. herpes is common, but there are several distinct differences between the two. Many people confuse genital warts with sores or blisters caused by a herpes infection, but different viruses cause them.
What Are Genital Warts?
Genital warts are caused by the human papillomavirus, otherwise known as HPV. HPV is the most common STD (sexually transmitted disease) in the United States; most people will contract some strain of the virus in their lifetime. Like other STDs, HPV is transmitted through intimate skin-to-skin contact, including vaginal, oral, and anal sex.
There are more than 150 types of HPV, and the different virus types range in severity. With most forms of HPV, the virus is asymptomatic and will go away on its own, without treatment. Certain strains of HPV, though, cause genital warts. Other strains can cause cancers of the cervix, penis, mouth/throat, anus, vagina, and vulva.
Genital warts caused by HPV appear as small bumps or groups of bumps. They can differ in size and appearance but are often flesh-colored, raised, and cauliflower-like. They can be removed like warts you would get elsewhere on your body. Genital warts can form on the vulva, penis, scrotum, thighs, lips, and around the mouth. Warts can also form on the walls of the vagina, on the cervix, and inside the mouth or throat, which can be more challenging to spot. Although the warts are usually painless, some people notice itching and bleeding during sex. After contracting HPV, it can take anywhere between six weeks and six months for genital warts to develop (if they develop at all). Occasionally, the virus remains dormant for years before genital warts develop.
Other types of HPV can increase the risk of cervical, penile, vulvar, vaginal, anal, and throat/mouth cancers. It often takes decades for the virus to cause cancer. These strains of HPV do not cause warts; most people don’t know they have the virus until they develop health problems. These types of HPV are passed from person to person in the same ways as the HPV strains that cause warts.
To prevent the transmission of any type of HPV, use condoms or dental dams when having vaginal, anal, or oral sex. Using them is not as effective in preventing HPV as it is in preventing other STDs, but it does help lower your chances of getting infected. Being in a monogamous relationship and knowing the sexual history of your partner also helps reduce the chances of getting HPV. It’s also important to have regular gynecological exams as part of your sexually active lifestyle. While a gynecological exam does not typically screen for STDs, a Pap smear can help doctors recognize abnormal cells on the cervix that can be caused by HPV. Early detection is critical: Once recognized, those cells can be removed to reduce cervical cancer risk. Be sure to ask your doctor about other STD tests or cancer screenings.
There is currently no cure for HPV, but the virus often clears up without treatment for people who get infected. Warts that develop can be removed just like warts on other body parts. The best thing to do is to prevent getting HPV by getting vaccinated. The vaccine protects against several types of HPV that cause warts and cancers. Thanks to the HPV vaccine, the rates of young people getting infected are dropping.
What is Herpes?
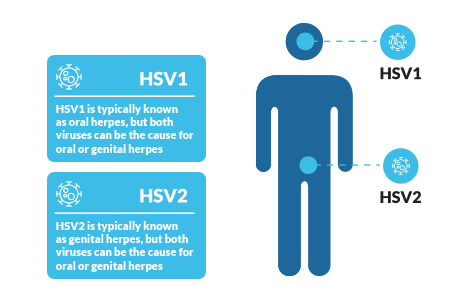
Herpes is an STD caused by one of two viruses: herpes simplex virus type-1(HSV-1) and herpes simplex virus type-2 (HSV-2). HSV-1 is typically known as oral herpes, the virus that can cause cold sores and fever blisters on or around the mouth. When people think of genital herpes, they are likely thinking of HSV-2. However, both HSV-1 and HSV-2 can cause either oral or genital herpes.
Herpes, like HPV, is prevalent in the United States: The CDC estimates that one in six people in the US has genital herpes and that more than half of the US population has oral herpes. Like HPV and other STDs, herpes is spread not only through intimate contact, including vaginal, anal, and oral sex, but also kissing and any other activity in which infected skin is exposed to a sensitive area, such as the genitals, mouth, and eyes.
Many people with herpes don’t have outbreaks or may not have an outbreak until years after getting infected. When they do develop, herpes sores look like blisters which then break and turn into painful ulcers. They can appear on or around the genitals, including the vagina, vulva, cervix, anus, penis, scrotum, butt, and thighs, as well as on the lips or around the mouth. The virus is most infectious when the sores are present, but you can still contract herpes from someone who has the virus but is asymptomatic or has never had an outbreak.


One in six people in the US has genital herpes, and more than half of the US population has oral herpes.
There is no cure for herpes, and the virus does not disappear. People with herpes have the virus for life. That being said, herpes is typically asymptomatic, except for periods when sores develop, referred to as outbreaks or flare-ups. Many people will experience fewer and fewer herpes symptoms as time passes, and the outbreaks will typically lessen in severity. Medication is also available to treat the symptoms and shorten the duration of outbreaks.
Genital Warts vs. Herpes
Different viruses cause genital warts and herpes. Herpes is not a type of HPV, nor is it caused by HPV, and HPV does not cause herpes sores or blisters. People infected with either HPV or herpes may not have any symptoms. Both viruses are spread through sexual and intimate skin-to-skin contact, so practicing safer sex and limiting the number of sexual partners is vital to prevent the spread of the virus. HPV can even be prevented with a vaccine. There is no cure for HPV or herpes once someone is infected, though treatments are available for both.

